这些天关于ARDS全球新定义(A New Global Definition of Acute Respiratory Distress Syndrome)的报道满天飞。
说实话,我看了不少翻译组的译文,觉得不是很满意,不如自己也梳理一下。LOGO:085101
1. 新定义的发布
新的定义将在ATS 2023年会的第4天(也就是5.24)作为当天小型研讨会(mini symposium)——“D16. ADVANCING THE SCIENCE OF ARDS AND ACUTE RESPIRATORY FAILURE” 的一个议题进行阐述、讨论(发布则是在大会的abstract册发布的)。
2. 新定义的全文
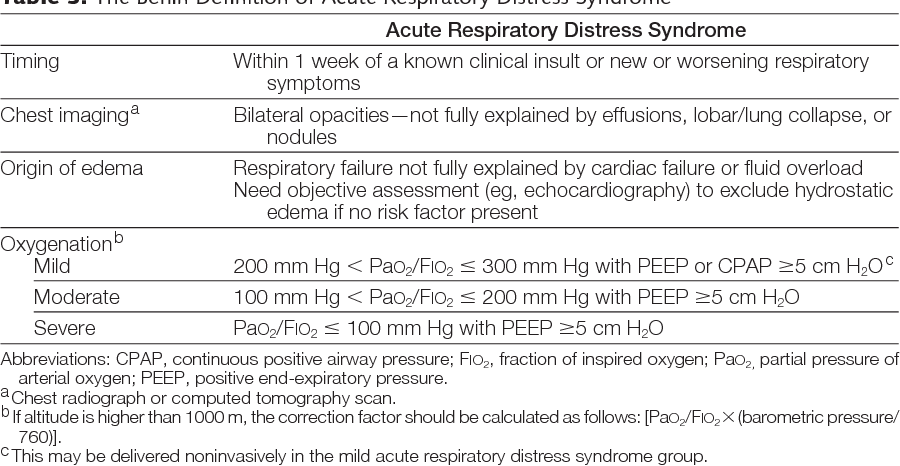
很可惜。目前大家拿到的就是这个摘要册里面的那些话,全部PDF就两页,如下图:


3. 新定义的背景
多说一句,实话实说,目前所有中文译文都令人极为不舒服—— 就知道抢发,翻译的太令人难受了。任何译文如果不能通顺阅读都是有毛病的,都要重译!
-
经鼻高流量氧疗(HFNO)已广泛用于严重低氧性急性呼吸衰竭,但这些患者不符合柏林定义;
-
经观察性研究和临床试验验证,指脉氧仪的SpO2/FiO2可作为ARDS的诊断标准;
-
胸部成像中究竟需要双侧还是单侧病灶(opacities)要进行重新讨论评价;此外,肺部超声可否作为胸部成像的补充也需要明确;
-
在医疗资源匮乏地区,因诊断(胸部X光、动脉血气分析)和治疗(正压通气)手段短缺,柏林定义的适用性受限。
4. 新定义的内容
基于以上(旧定义的)不足,新定义经过多轮多国专家的讨论提出了新4条:
-
(非插管的)使用最小流速≥30 L/min的HFNO,或使用呼气末压力至少为5cmH2O的NIV/CPAP无创通气纳入ARDS;
-
以PaO2/FiO2≤300mmHg或SpO2/FiO2≤315mmHg且SpO2≤97%来识别低氧血症;
-
仍保留胸部X光或CT“双侧病灶“”的标准,并添加超声诊断(需经良好训练);
-
医疗资源有限情况下,无需PEEP、氧流量或特定的呼吸支持设备来诊断ARDS。
5. 新定义的评价
这个我应该可以写一篇英文讨论稿的,在这里暂不发表,以免被那个了。
-
新定义确实扩大了柏林定义的范畴,可能会有助于ARDS患者的早期识别及及时启动救治(我猜测,纳入非插管的HFNO以及无创通气的标准,主要还是基于新冠大流行期间大量重症COVID的诊疗实践获得的教训—COVID-19 大流行导致 ARDS 发病率增加了 10 倍或更多!这一点而言是非顺应形势的及时更新)
-
目前已有的资料没有提及原柏林定义是否继续沿用,最重要的是原定义的发病时间以及轻、中、重分型是否沿用,但问题是因为柏林定义有PEEP的限制,这显然跟新定义冲突—新定义会不会取消这些限制而直接按轻、中、重分型;此外,脉氧指数SpO2/FiO2是否也要分级?我想大概率是不会了。

-
任何定义都应该将复杂问题简单化,作为一种至今发病原因复杂、病理生理机制不明确、无特异性治疗手段的综合征,目前“扩增”的定义中似乎没有一项是可以针对某特定病因、病机和治疗而去的,从这一点看,实际也就不存在关键意义的定义提升,甚至增加了诊断的负担。换句话说,该定义无形中也会增加假阳性病例——实际并非ARDS但因实施了HFNO以及大量因缺乏诊疗设施设备而诊断ARDS者。
-
由于新定义全文和详实的阐述并没发表,我们没法进一步详细阐述。但新定义至少也没有给到与表型、分型以及生物标志物等核心内容的更新,这是有点“临床不友好”了。
ARDS定义的变化,很像近年来脓毒症定义的变化,要么增加了太多的细枝末节的约束,要么就是敏感性、特异性、假阳性、假阴性的跳跃,这种更新对重症医学的发展究竟是有益呢还是无益呢?
-
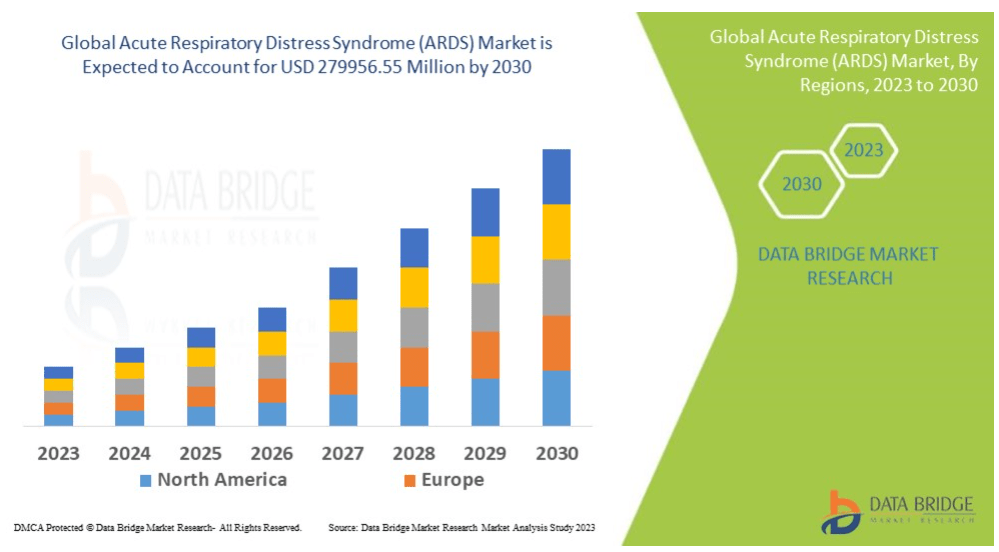
国际专家们怎么就把这么一个仍存在显著争议的概念当成“全球”定义了?(我看到一份国际市场研判报告,里面说从2023到2030,ARDS的全球市场那是突飞猛进的,我不怀好意地感觉新定义将会带来HFNO,乃至超声厂商的推动。是的,任何国际定义和指南的更新一直都伴随着点啥)
-
6. 其他文献讨论
尽管新定义的正文以及详细的组织阐述未发表,但近期几篇在大刊上发表的文献可以说已经和上述定义遥相呼应,并给出了我们想要的部分“评价”,值得一谈。
-
Acute respiratory distress syndrome in adults: diagnosis, outcomes, long-term sequelae, and management.
Gorman EA, O’Kane CM, McAuley DF(也是新定义的署名作者之一).
Lancet. 2022 Oct 1;400(10358):1157-1170. doi: 10.1016/S0140-6736(22)01439-8.
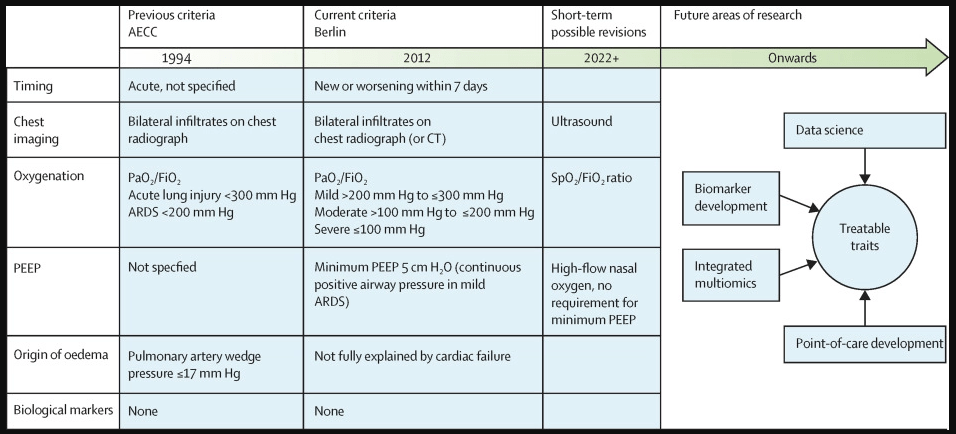
看到没有,McAuley DF教授已经就诊断更新给出了路线图,在文中他更是写到:
(胸片的单双侧病灶)Chest radiographic criteria for ARDS are recognised to have suboptimal interobserver reliability and are under-recognised in clinical settings.22 In research settings tools have been investigated to improve the reliability of ARDS diagnosis. The Radiographic Assessment of Lung Oedema score, using a visual assessment of four quadrant consolidation and infiltrate density, has been shown to have good intraobserver reliability and high diagnostic accuracy for ARDS.23 A similar visual assessment score has been shown to correlate with important clinical outcomes including mortality and duration of intensive care unit stay.24 Artificial intelligence technology (using deep convolutional neural networks that can be trained to recognise findings on imaging), such as the ARDS Detection Tool, is another tool that has been shown to accurately identify bilateral airspace consolidation consistent with ARDS in research settings but requires further validation before clinical use.25
(超声)Ultrasound imaging is emerging as a safe, inexpensive, bedside tool for the evaluation of ARDS although the need for training is recognised to be essential before this tool can be implemented as a diagnostic imaging modality for pulmonary infiltrates.
(脉氧指数)A ratio between oxygen saturation, measured by pulse oximetry, and fraction of inspired oxygen (SpO2/FiO2) is an attractive alternative to a ratio between partial pressure of arterial oxygen and FiO2 (PaO2/FiO2) ratio due to its availability and safety. These simple bedside tools could be useful in resource-limited settings, and outside the traditional intensive care unit.26, 27, 28 Evidence from retrospective analysis supports the ability of the SpO2/FiO2 ratio to predict outcomes in patients with ARDS.26 In resource-limited settings, in which mechanical ventilation, blood gas analysis, and chest imaging might not be available, the Kigali modification using the SpO2/FiO2 ratio and lung ultrasound has been suggested and has been useful to evaluate ARDS.29, 30 Additionally the Kigali modification removes the requirement for positive end expiratory pressure (PEEP) as ventilator resources might not be available.29
(超声与脉氧指数的不足)Lung ultrasound and SpO2/FiO2 ratio have limitations as diagnostic tools in ARDS. Lung ultrasound could overestimate ARDS. Vercesi and colleagues31 reported a high rate of false positives when comparing the Kigali modification with the Berlin criteria for ARDS in a single centre observational study in the Netherlands. The high false positive rate was attributed to the sensitivity of lung ultrasound in detecting interstitial infiltrates and consolidative changes.32 In addition, pulse oximetry could cause disparities in the identification of occult hypoxaemia due to skin colour.33 Further prospective studies are required to determine optimal SpO2/FiO2 thresholds for severity, which should account for differences in race and ethnic origin.
(正压通气)The requirement for positive-pressure ventilation means many patients with non-cardiogenic acute hypoxaemic respiratory failure and bilateral infiltrates cannot meet the definition of ARDS, despite having similar biological characteristics to patients with these characteristics on positive-pressure ventilation. Given the increasing use of high-flow nasal oxygen, which might deliver low levels of PEEP as one of its physiological benefits,34 there is interest in including high-flow nasal oxygen in future definitions of ARDS.35 A modification to include high-flow nasal oxygen in the ARDS definition would allow early identification of patients with ARDS and facilitate recruitment to clinical trials at an earlier timepoint in the clinical course of ARDS. There are potential limitations of this modification. For instance, in a single centre prospective study of 148 patients, PaO2/FiO2 was found to vary substantially after a change in respiratory support from high-flow nasal oxygen to invasive ventilation.36 Furthermore, Ranieri and colleagues37 showed that patients fulfilling ARDS criteria on high-flow nasal oxygen who transition to invasive mechanical ventilation might have lower mortality rates than patients on non-invasive ventilation who transition to invasive mechanical ventilation.
-
Newly Proposed Diagnostic Criteria for Acute Respiratory Distress Syndrome: Does Inclusion of High Flow Nasal Cannula Solve the Problem?
Liufu R, Wang CY, Weng L, Du B.
J Clin Med. 2023 Jan 29;12(3):1043. doi: 10.3390/jcm12031043.
杜斌老师在今年1月份的文献中就HFNC可否作为ARDS的诊断标准做了一番阐述。如同上述,正是由于新冠救治的文献研究,HFNC 被 Surviving Sepsis 运动、ERS 和NIH)的指南推荐,尽管也存在相互矛盾的结果 。HFNC 在 AHRF 管理中的应用越来越多,这种扩大被认为有助于及时诊断 ARDS 并在更广泛的患者群体中进行,例如无论是否需要气管插管和/或正压通气但接受了一定程度呼吸支持的轻度至中度肺损伤患者。此外,ARDS 的这一扩展定义也将有助于临床实践中的患者管理和临床研究中的患者招募。但 Inclusion of HFNC真的能Solve the Problems with the Berlin Definition吗?
核心理由是—— 不能根据治疗的干预措施来诊断或定义,确实如此!简言之,你不能把一个接受了开颅手术的患者都定义为脑水肿。或者接受皮质醇治疗的患者都定义为风湿一样(杜老师举的例子是:让我们假设一名 AHRF 患者接受清醒体外膜肺氧合 (ECMO) 治疗,但呼吸室内空气。该患者不符合现行的柏林定义或提议的 ARDS 修改定义。这样,我们是否应该对柏林定义提出另一种修改,以包括接受 ECMO 治疗的患者?)—— If we want to define a disease or clinical syndrome according to any therapeutic interventions and/or a minimal response to a therapeutic intervention, it should be based on two premises: first, all patients with the disease/syndrome should have the same chance of receiving the specified therapeutic intervention; second, all clinicians may comply to the same strategy with regard to the specified therapeutic intervention (e.g., PEEP setting). When applying the above two premises to patients with ARDS, this means that all patients with ARDS should have the same chance of receiving the same respiratory support (including HFNC, NIV, and IMV), and all intensive care physicians should set the same PEEP level in the same patient.Unfortunately and obviously, none of the above premises is true.
希望以上的梳理能够让我们在接受新定义之前和之后能有更多的考量。
本文荟萃自公众号: 重症危通社,只做学术交流学习使用,不做为临床指导,本文观点不代表数字重症 ICU.CN立场。







 微信扫一扫
微信扫一扫